 
It helps me to simply remember that these eyes have more than just microaneurysms but less than any of the criteria in the 4:2:1 rule (described below). More than just micro aneurysms (with or without cotton-wool spots, venous beading, or IRMA) but less than the 4:2:1 rule Moderate nonproliferative diabetic retinopathy (Moderate NPDR) Moderate NPDR Proposed Diabetic Retinopathy Severity Level These patients can be followed every 12 months. All things considered, this is pretty low risk. In other words, a diabetic patient with no retinopathy has a <1% chance of developing PDR and a diabetic patient with a rare MA/DBH has a <5% chance of progressing to PDR in the next four years. 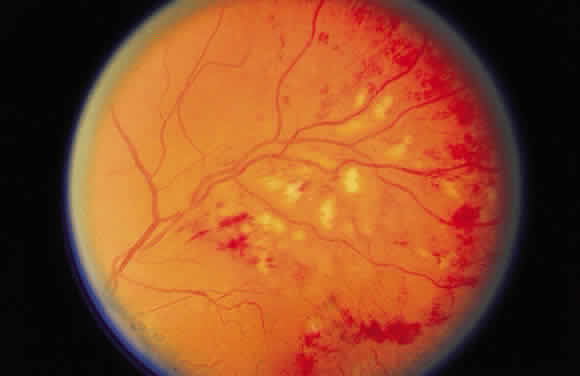
However, the Wisconsin Epidemiological Study of Diabetic Retinopathy (WESDR) did include these individuals in its study, and found that the rate of progression to PDR after four years was less than 1% for both young and older patients with no diabetic retinopathy, compared to 4.1% in younger patients with a rare microaneurysm and hemorrhage and even less in older patients with these findings. Both have a very low risk of progressing to PDR in fact, the Early Treatment Diabetic Retinopathy Study (ETDRS) did not examine those with no retinopathy nor mild NPDR. In reality, there is not much difference in risk between diabetic eyes with no retinopathy and those with mild retinopathy. Mild nonproliferative diabetic retinopathy (Mild NPDR) No retinopathy and mild NPDR Proposed Diabetic Retinopathy Severity Level After nervously searching Google in the physicians workroom for the diabetic retinopathy grading scale more often than I care to admit, I have decided to summarize the classification criteria for diabetic retinopathy, at least in a way that makes sense to me. Intraretinal hemorrhages similar to those found in the retinopathy associated to blood dyscrasias could be an association with SARS-CoV-2 in the context of a coagulopathy induced by the infection.ĬOVID-19 SARS-CoV-2 intraretinal hemorrhages novel coronavirus ophthlamology.Accurately grading diabetic retinopathy can be a significant challenge for beginning ophthalmology residents. After 1 month of the COVID-19 treatment, fundus examination improved and fluorescein angiography demonstrated no diabetic retinopathy signs, no retinal vasculitis and no significant delay in arterial or venous filling. Fundus examination revealed bilateral venous stasis and dot and blot intra-retinal hemorrhages preceding the diagnosis of COVID-19 in a patient with mild respiratory symptoms that progressed within a few days to a severe respiratory distress. We report here the first case of a patient with bilateral unusual dot-blot retinal hemorrhages and retinal venous dilation who presented shortly thereafter a PCR-proven COVID-19.Ī 59-year-old woman presented with a 7 days history of blurred vision in both eyes. As the pandemic is spreading and the whole picture is yet unknown, ophthalmologists should be aware of unusual ocular presentations of COVID-19 since they could precede the development of severe respiratory distress. There have been anecdotal reports of ocular manifestations in the Coronavirus Disease 2019 (COVID-19).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
